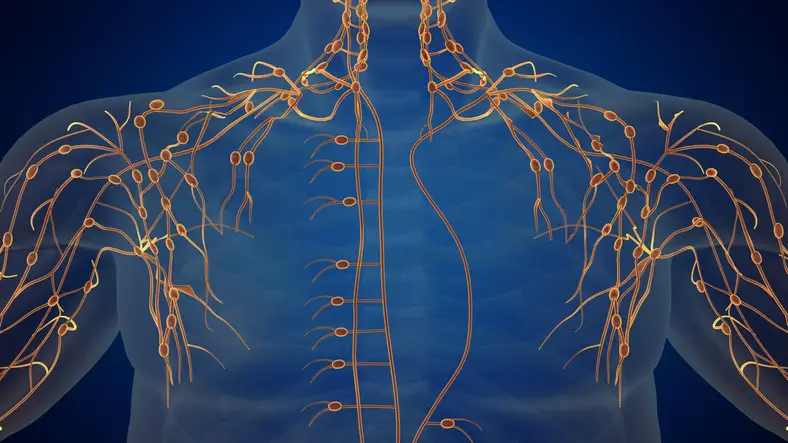
A common, but under-discussed symptom of breast cancer treatment is lymphedema. Those who have had their lymph nodes removed or undergone radiation therapy have a higher risk of experiencing long-term lymphedema symptoms. Because there are so few conversations had about this side effect, it can catch patients off guard when it arises. This issue is compounded by the fact that doctors can’t predict which patients will end up developing it.
While lymphedema symptoms can arise during or after any type of cancer treatment, it’s especially common for breast cancer patients. Different studies present a wide range of numbers regarding how many breast cancer patients experience lymphedema, but according to the Journal of Clinical Oncology as many as 83% of breast cancer patients can experience it. Black women are especially likely to develop lymphedema following treatment for breast cancer compared to white women. Black women have a 3.85-fold increased risk.
Lymphedema can present immediately after treatment or can arrive after years, although most cases occur in the first 18 months. To better understand what lymphedema is, what the symptoms are like, and how to treat those symptoms, keep reading.
Evidence-based guidance powered by NCCN Guidelines®
Personalized treatment plans shaped by the latest oncology standards—tailored to your diagnosis.
Get started
View your personalized treatment plan in the Outcomes4Me app
Use your diagnosis to unlock personalized NCCN Guidelines®-aligned recommendations.
Continue in app
What is lymphedema?
Lymphedema is a medical condition caused by disruption or damage that occurs to someone’s lymphatic structures (like lymph nodes or lymph vessels). Essentially this system cleans, filters, and processes protein-rich fluid. When that fluid becomes stagnant, it can back up and lead to tightness, swelling, and discomfort.
For more extreme cases, fibrosis can occur which is hardening of the tissue, there can be loss of skin integrity that leads to open wounds, and you can lose limb function. Breast cancer patients are more likely to experience swelling in their hands, arms, breasts, and the side of the body they received treatment on.
As lymphedema symptoms advance, the need for treatment can increase and the chance of dangerous complications like bacterial infections that can be life-threatening.
How does breast cancer treatment lead to lymphedema?
The lymphatic system works like a machine and each lymph vessel and lymph node is an integral part of the machine that keeps it working correctly. When you take away or damage a part of a machine, it may still function but not quite as well as it used to. Each adult has about 600 to 700 lymph nodes in their body, even missing just one can affect the entire system and lead to lymphedema.
Certain breast cancer treatments can lead to damaging or removing parts of the lymphatic system. Here’s a closer look at those treatments:
- Lymph node biopsy. Because breast cancer can spread via the lymphatic system, some patients receive a sentinel node biopsy. This biopsy removes the lymph node closest to the tumor and can involve removing up to six nodes.
- Lymph node dissection. This type of dissection occurs when most or all of the lymph nodes in the armpit are removed when cancer is indicated in lymph nodes through imaging or biopsy.
- Radiation therapy. Because radiation therapy can affect all cells it comes into contact with, this treatment can damage the lymph nodes’ ability to function properly and can create scar tissue in lymph vessels that makes it more difficult for the thick lymph fluid to move along.
What are the signs of lymphedema?
How someone’s body reacts to lymphedema can vary, but the following side effects are common. Knowing what side effects to look out for is key so you can alert your care team that you may need to pursue treatment for your lymphedema symptoms.
- Aching. Some people experience a dull ache that comes and goes.
- Heaviness. Your arm or hand might feel heavier than the other side of your body. You may also experience a heaviness or fullness in your breast or around your ribcage on your cancer side.
- Tingling or numbness. An early sign of lymphedema is a tingling or numbness anywhere along the affected area—including the armpit.
- Non-visible swelling. Swelling can be subtle, so keep an eye out for watches, jewelry, or clothing feeling a bit tighter than normal.
- Itching or tightness of the skin. Skin can look or feel tight or start to itch when swelling occurs.
Personalized support for real care decisions
Understand your diagnosis, explore clinical trials, and track symptoms--all in one place.
Get started
Compare treatments, prepare for appointments, and track side effects—all in the app
Built for your diagnosis, Outcomes4Me gives you the tools to make confident, informed decisions—right when you need them.
Continue in app